Researchers around the world have begun linking dementia and diabetes, calling Alzheimer’s “diabetes type 3”, though it remains a new, unofficial term that many professionals still consider controversial. When analyzing both diseases separately, similarities noticeably surface, causing this hypothesis to arise.
It is first and foremost important to understand the difference between dementia and Alzheimer’s. The former is a general term grouping diverse symptoms that affect abilities such as memory and behaviour. Alzheimer’s is its most common form, being a progressive neurodegenerative disorder that primarily affects memory and cognitive abilities, such as coordination, daily functioning and attention. This degeneration is caused by the death of neurons which are specialized brain cells that are essential to transmitting information throughout the body. There are two main reasons for the death of neurons: amyloid plaques and neurofibrillary degeneration.
Amyloid plaques are created by an unusual accumulation of beta-amyloid protein between neurons. This protein is naturally found in the brain and becomes problematic when it accumulates, because it prevents neurons from properly functioning by surrounding them, eventually leading to their death and accelerating the disease’s symptoms. In fact, beta-amyloid begins silently settling in the brain 20 to 30 years prior to the first signs of cognitive decline.
Neurofibrillary degeneration, on the other hand, is caused by the accumulation of the protein TAU, which plays a crucial role in the brain. Situated inside the neuron, this protein maintains and stabilizes its skeleton to allow communication with other neurons. In the case of a cognitive disease, the TAU protein separates from the skeleton and builds up inside neurons, ceasing connections and leading to their deaths.
To connect both diseases, it is also crucial to understand diabetes. Many forms of this disease exist, though only one is pertinent in this hypothesis, notably type 2. Insulin, produced by the cells of the pancreas, moves glucose from the blood to skeletal muscle cells and liver cells to create energy. Diabetes type 2 is characterized as a resistance to insulin, meaning the body can create the necessary insulin, but cannot use it properly. Thus, the blood sugar levels increase and lead to health problems related to nerves, the heart, the kidneys, the eyes, etc. This variant of diabetes is not hereditary and is developed through unhealthy habits.
The link between these diseases is based on research proving that type 2 diabetes patients are more prone to eventually having Alzheimer’s. Two similarities could explain this connection.
First, various cardiovascular problems are risk factors for both type 2 diabetes and Alzheimer’s. These cardiovascular problems include, but are not limited to, obesity, heart disease or a family history of heart disease, circulatory problems, high cholesterol, high blood pressure, and weakened blood vessels. Secondly, studies have found that glucose tends to be used incorrectly in the brain of an individual suffering from Alzheimer’s disease, in a similar manner to type 2 diabetes. The death of neurons caused by amyloid plaques and neurofibrillary degeneration interferes with the brain’s capacity to interpret messages, including the necessary quantity of insulin for good bodily function. Additionally, by preventing the insulin receptors from understanding transmitted information, the altered production of insulin leads receptors to become insensitive to it.
Umeå University in Sweden confirmed a connection between diabetes and Alzheimer’s during a study in 2024. Two groups were gathered, both formed of people aged between 66 and 72 years old, one of which included relatively healthy people and the other people with type 2 diabetes. Each group received a glucose infusion over a four-hour period. The researchers found that those who were in healthy condition underwent a decrease in beta-amyloid, while those with diabetes did not experience any change in the levels of this protein, thus increasing the risks of an accumulation in the brain and the creation of amyloid plaques.
Calling Alzheimer’s “diabetes type 3” implies that it is a separate form of diabetes situated in the brain, when it is truly not that simple. The term is not yet official or recognized in the medical field, although it contributes to much controversy among professionals, as many hesitate to associate the two diseases despite the similarities. Doctor Maï Panchal explained in French, “It is important to differentiate between a disease caused by an accumulation of malformed proteins in the brain, and a pathology linked to an accumulation of sugar in the blood.”
It is also important to acknowledge that both diseases are managed differently. For diabetics, a diet rich in fiber and low in sugar is recommended to mitigate the effects of the disease, but this solution does not apply to improve the symptoms of Alzheimer’s.
Written in collaboration with Mila Logan.
BIBLIOGRAPHY
PHOTO GETTY IMAGES. (2021). Illustration de plaques amyloïdes (orangées)
accumulées sur des neurones dans le cerveau, l’une des plus importantes
caractéristiques de la maladie d’Alzheimer. [image en ligne]. Le mystère des plaques
amyloïdes,LaPresse. https://www.lapresse.ca/actualites/sciences/2021-05-16/maladie-d-alzheimer/le-mystere-des-plaques-amyloides.php
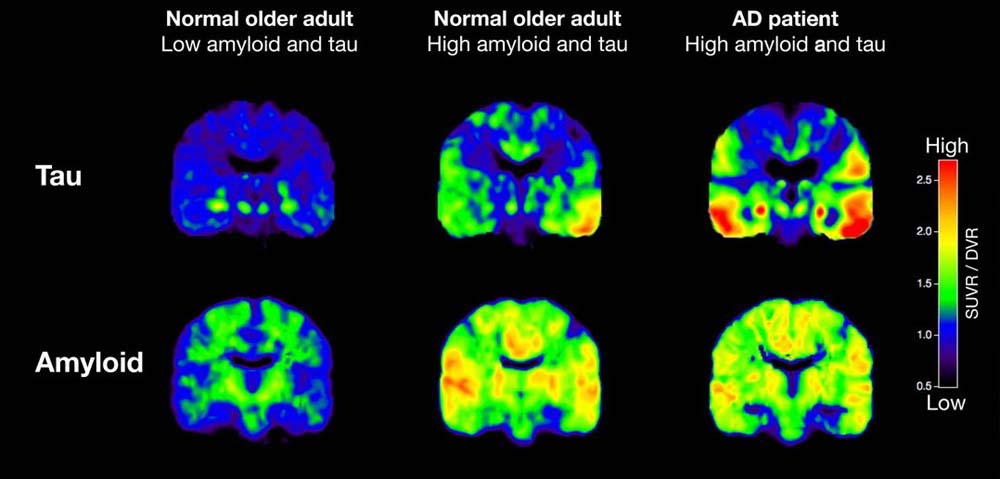
PsyPost. (s. d.). Amyloid and Tau Imaging. [image en ligne]. PACIFIC BRAIN
HEALTH CENTER. https://www.pacificneuroscienceinstitute.org/brain-health/services/brain-imaging/
Livre et article papier:
- Stanislas Dehaene. (2021). F ACE À F ACE AVEC SON CERVEAU (7381-5702-X,
volume 1). Odile Jacob.
- Raphaëlle Derome. (2024, juin) Nouveaux Traitements: à quoi s’attendre. Québec
Science, pages 16-17.
- Auteur inconnu. (2024, juin) Maladie d’Alzheimer: voir ses traces dans le cerveau.
Québec Science, page 18.
- Raphaëlle Derome. (2024, juin) Au-delà des médicaments. Québec Science, pages
19-21.
Sites Web:
- (https://www.fondation-alzheimer.org/dictionnaire/)
- Lynda De Widt. (25 octobre 2017). What is the link between Alzheimer’s and Type 3 diabetes?. Mayo Clinic| News Network. https://newsnetwork.mayoclinic.org/discussion/researchers-link-alzheimers-gene-to-type-iii-diabetes/
- Manon Duran en collaboration avec Dre Maï Panchal (20 mai 2022) Qu’est-ce que le diabète de type 3? Santé Magazine https://www.santemagazine.fr/sante/maladies/maladies-neurologiques/maladie-d-alzheimer/quest-ce-que-le-diabete-de-type-3-919148#:~:text=Alzheimer%2C%20nous%20%C3%A9claire.-,Qu’appelle%2Dt%2Don%20diab%C3%A8te%20de%20type%203%20%3F,du%20glucose%20dans%20le%20cerveau
- Équipe de la Sun Life. (11 novembre 2024). Diabète de type 1 et de type 2: quelle est la différence? .Sun Life. https://www.sunlife.ca/fr/tools-and-resources/health-and-wellness/preventing-and-treating-illness/diabete-de-type-1-ou-de-type-2-quelle-est-la-difference/
- Élyanthe Nord. (28 Juillet 2021). Diabète de type 2 traité par une insuline basale. LE MÉDECIN DU QUÉBEC. https://lemedecinduquebec.org/archives/2021/8/diabete-de-type-2-traite-par-une-insuline-basale-un-systeme-de-surveillance-en-continu-de-la-glycemie-est-il-utile/
- La maladie d’Alzheimer, Causes, mécanismes biologiques, symptômes, diagnostic et traitements. (22 novembre 2024). Institut du Cerveau. https://institutducerveau.org/fiches-maladies/maladie-dalzheimer
- Diabète de type 2. Gouvernement du Canada. (30 novembre 2023). https://www.canada.ca/fr/sante-publique/services/maladies/diabete-type-2.html#:~:text=Type%201%20%3A%20le%20corps%20ne,insuline%20correctement%20pendant%20la%20grossesse
- La maladie d’Alzheimer. (22 novembre 2024). Institut du Cerveau. https://institutducerveau.org/fiches-maladies/maladie-dalzheimer
- Possible explanation for link between diabetes and Alzheimer’s. (14 août 2024)Journal of Alzheimer’s Disease. https://www.iospress.com/news/possible-explanation-for-link-between-diabetes-and-alzheimers
- Étienne Aumont, (25 octobre 2022). Non, l’Alzheimer n’est pas un type de diabète. L’actualité https://lactualite.com/sante-et-science/non-lalzheimer-nest-pas-un-type-de-diabete/
- La différence entre la maladie d’Alzheimer et les autres troubles neurocognitifs. (s.d.). Société Alzheimer. https://alzheimer.ca/fr/au-sujet-des-troubles-neurocognitifs/quest-ce-que-la-maladie-dalzheimer/la-difference-entre-la
- Diane Sievert. (26 juin 2023).Alzheimer’s Vs Dementia – What Is The Difference?. UCLA David Geffen School of Medecine. https://medschool.ucla.edu/news-article/alzheimers-vs-dementia-what-is-the-difference#:~:text=In%20summary%2C%20dementia%20is%20an,own%20distinct%20causes%20and%20characteristics
- Journal Of Diabetes Science And Technology. (Novembre 2008). Alzheimer’s Disease Is Type 3 Diabetes- Evidence Reviewed. National Library of Medecine. https://pmc.ncbi.nlm.nih.gov/articles/PMC2769828/
- Mayo Clinic Staff. (s. d.). Type 1 diabetes. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/type-1-diabetes/symptoms-causes/syc-20353011
- Diabetes and dementia. (s. d.). Alzheimer Society. https://alzheimer.ca/en/about-dementia/how-can-i-prevent-dementia/diabetes
- Le dépistage génétique et la maladie d’Alzheimer. (s. d.). Société Alzheimer. https://alzheimer.ca/fr/au-sujet-des-troubles-neurocognitifs/quest-ce-que-la-maladie-dalzheimer/le-depistage-genetique-et